Regenerative endodontic procedures can be defined as biological procedures designed to replace damaged structures, including dentin and root structures, as well as cells of the pulp-dentin complex.
This exciting new phase of dentistry is continually evolving and becoming more predictable. Below is a recent case.
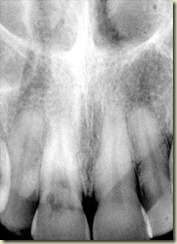
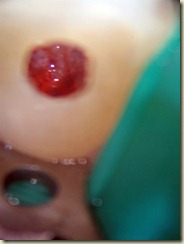
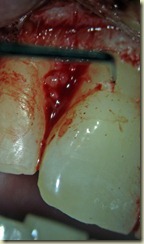
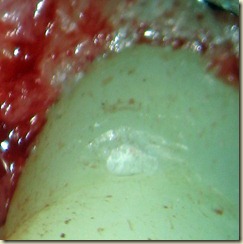
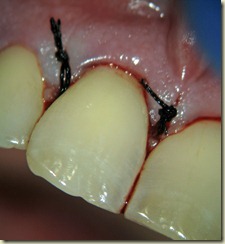
8 year old male presents for evaluation and treatment. Recent dental history includes traumatic episode, 2 weeks prior. Patient had the incisal 
Diagnostic Testing:
#8: Adequate response to cold; no pain on percussion or palpation. WNL.
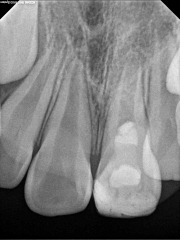
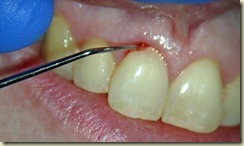
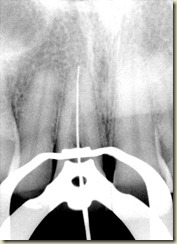
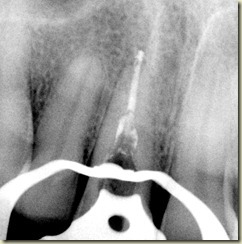
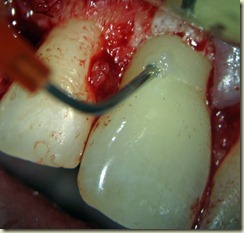
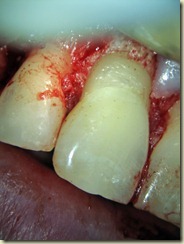
#9: No response to cold; very sensitive to percussion and palpation. 3+ mobility, depressible. Purulent drainage from buccal sulcus. Open Apex (incomplete root formation)
Dx: Necrotic #9
Treatment options include: Regenerative Endodontics, One-Step Apexification, or Extraction.
After discussing treatment alternatives with the parents and guarded prognosis, we decided to initiate root canal treatment and medicating the canal space on initial visit.
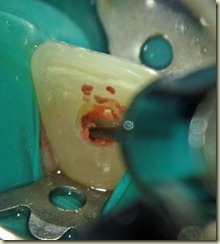
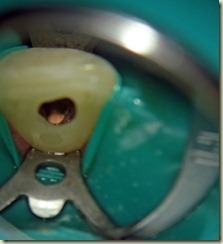
Local Anesthesia administered, tooth accessed via rubber dam isolation. Working length established of 22mm. Canal instrumented to size 100. Copious Irrigation with NaOCl; Ten min soak with
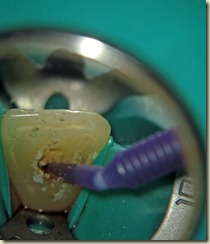
NaOCl. Canal dried. Copious Irrigation with Chlorihexidine .12%. Ten minute soak with Chlorihexidine .12%. Intracanal medicament of Calcium Hydroxide + Chlorihexidine placed using lentulospiral and appropriate sized pluggers. Access sealed permanently with composite resin.

At 2 week follow-up, evaluation revealed:
#9: No pain on percussion or palpation. No mobility. No purulent Discharge. Periodontal probing depths all within normal limits.
Decision made to proceed with Regenerative Endodontic Procedure with the goal of stimulating local stem cells to re-inhabit canal space and continue root formation for much improved long-term prognosis
Visit 2:Local Anesthesia (Carbocaine 4% without epinephrine) administered. Tooth accessed via rubber dam isolation. Calcium Hydroxide removed with Hand and Rotary files. Irrigation with .12% Chlorihexidine. 10 min soak with .12% Chlorihexidine. Canal Dried.
Size 100 file advanced 2-3 mm beyond apex to induce bleeding. Canal filled with blood. Waited 20 min for clot formation. 3 mm of MTA placed over clot. Access restored permanently with composite resin.
UPDATE (MAY 2011)
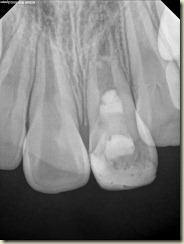
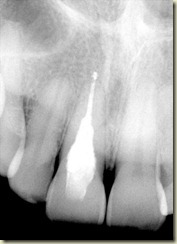
Below is a radiograph from the 6 month follow-up taken in September of 2010. At this point, the patient has no symptoms or pain in the area. In addition, all periodontal probing depths are WNL.
No real changes noted on the 6 month radiograph.
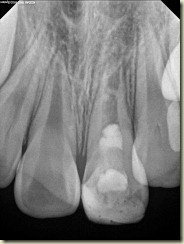
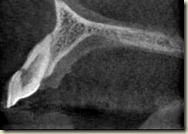
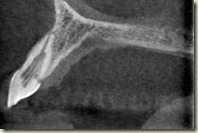
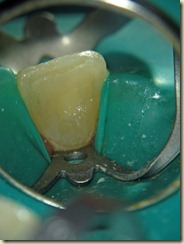
Below are two radiographs taken at the 1 year follow-up (April 2011)
1 year radiographs show some calcification within the canal. Apical width appears narrower than pre-operative radiograph, however still not formed fully. Patient still has no pain or symptoms. The periodontal probing depths are normal. While this is a newer aspect of endodontics, the few literature examples demonstrate that apical closure and root formation can take upward of 24 months. More details to follow…